Anxiety disorders form the most common class of mental disorders, with one in seven adults suffering from an anxiety disorder in any year: 14.4% in Australia and 14.8% in New Zealand. SAD is the most prevalent anxiety disorder, followed by general anxiety disorder and panic disorder/agoraphobia. Anxiety disorders are more common in women than men and in people who are separated, divorced or widowed, less educated or unemployed. Demographic status may be both a consequence and a cause of anxiety disorders.
Social Anxiety Disorder (SAD) has an early age-of-onset – usually between ages 13 and 15 and is often chronic. More than 90% of individuals with the disorder report impairments such as dropping out of school, reduced productivity at work, reduced socioeconomic status, and reduced quality of life. Despite the marked impairment, few people receive treatment, partly due to the core of the condition itself: the fear of social situations makes this population extremely hesitant to consult with healthcare professionals. However, anywhere from one-third to two-thirds respond to treatment. Evidence suggests that with lifetime SAD, approximately one in five ever obtained treatment. Among these, cumulative probability of receiving treatment regarded as helpful after seeing up to seven professionals was 92.2%. However, only 30.2% persisted this long, resulting in 65.1% ever receiving treatment perceived as helpful.
Implications for Clinical Practice
It may be important to align expectations of both practitioners and patients that more than one episode of treatment may be needed to achieve change that is considered helpful.
SSRI and SNRI are considered helpful treatments for social anxiety disorder. Often the improvement that is possible is a reduction in anxiety of 50-80%. It is important to explain to the patient that higher doses are required to treat anxiety than are required for depression. Very often patients will state that Medication A failed to help but the dose was not pushed up sufficiently. One of the main reasons patients stop their medication is due to sexual side-effects. It is helpful to open the communication regarding this by mentioning it to patients when they first start on these medications.
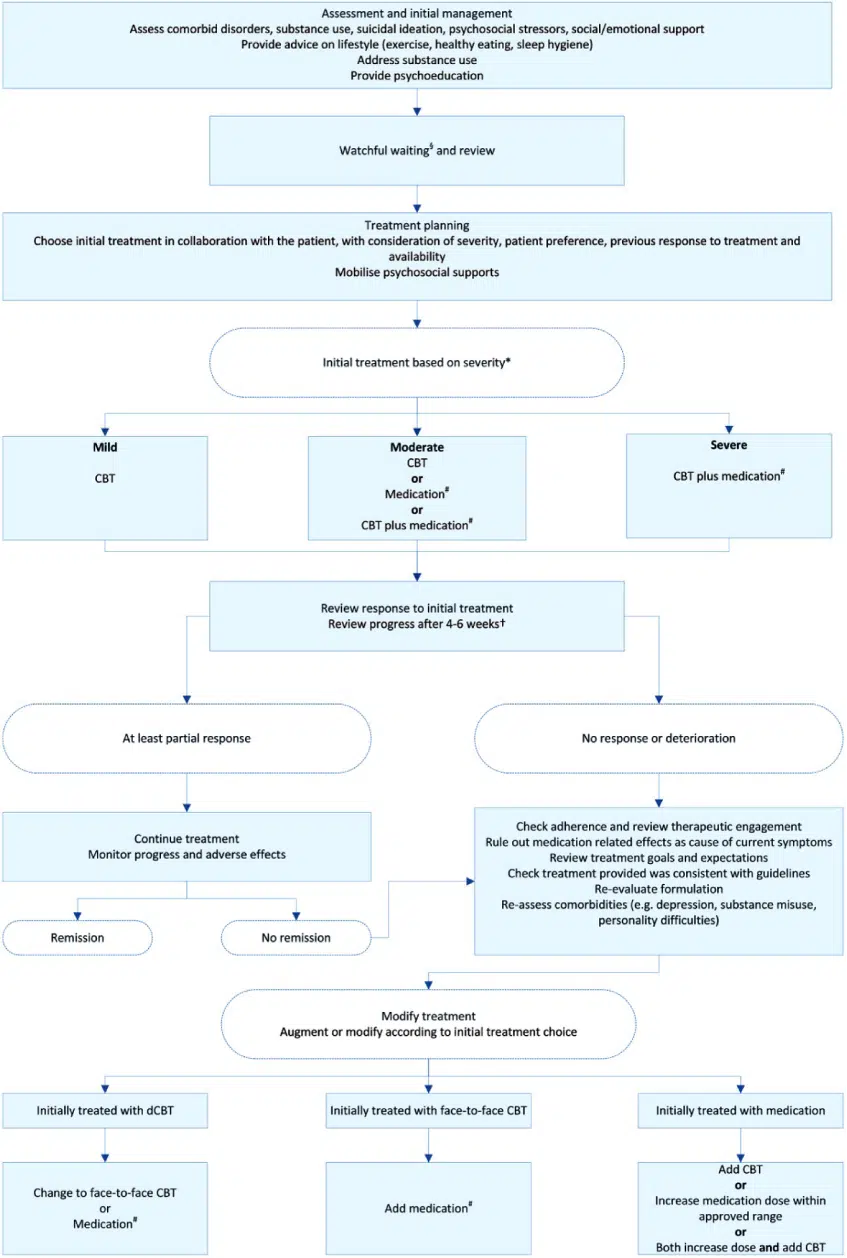
It is also useful to mention that use of anti-depressants can work synergistically with the required psychological treatments such as CBT, exposure therapy and response prevention. Patients need to know that the reduced anxiety from use of medication can enable them to engage with psychological treatments more effectively (See Figure 1; Australian & New Zealand Journal of Psychiatry 2018).
Co-occurring disorders with SAD include all other anxiety disorders, depression and substance use disorder. With more severe social anxiety disorder co-occurring illness is the rule rather than the exception. It is also useful to bear in mind that there can other differential diagnoses including Autism spectrum disorder and paranoia causing what appears to be symptomatic social anxiety disorder.
Figure 1: Overview of the management of anxiety disorders.
Conclusions
Most individuals with SAD do not receive any treatment. Among those who do, the probability that people treated for SAD obtain treatment they consider helpful increases considerably if they persist in help-seeking after earlier unhelpful treatments.
References
WHO World Mental Health Survey Collaborators (2022). Perceived helpfulness of treatment for social anxiety disorder: findings from the WHO World Mental Health Surveys. Social psychiatry and psychiatric epidemiology, 57(10), 2079–2095. https://doi.org/10.1007/s00127-022-02249-3
Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for the treatment of panic disorder, social anxiety disorder and generalised anxiety disorder (2018) Australian & New Zealand Journal of Psychiatry, 52:12, 1109-1172